Nursing Homes and the Risk of Candida Auris
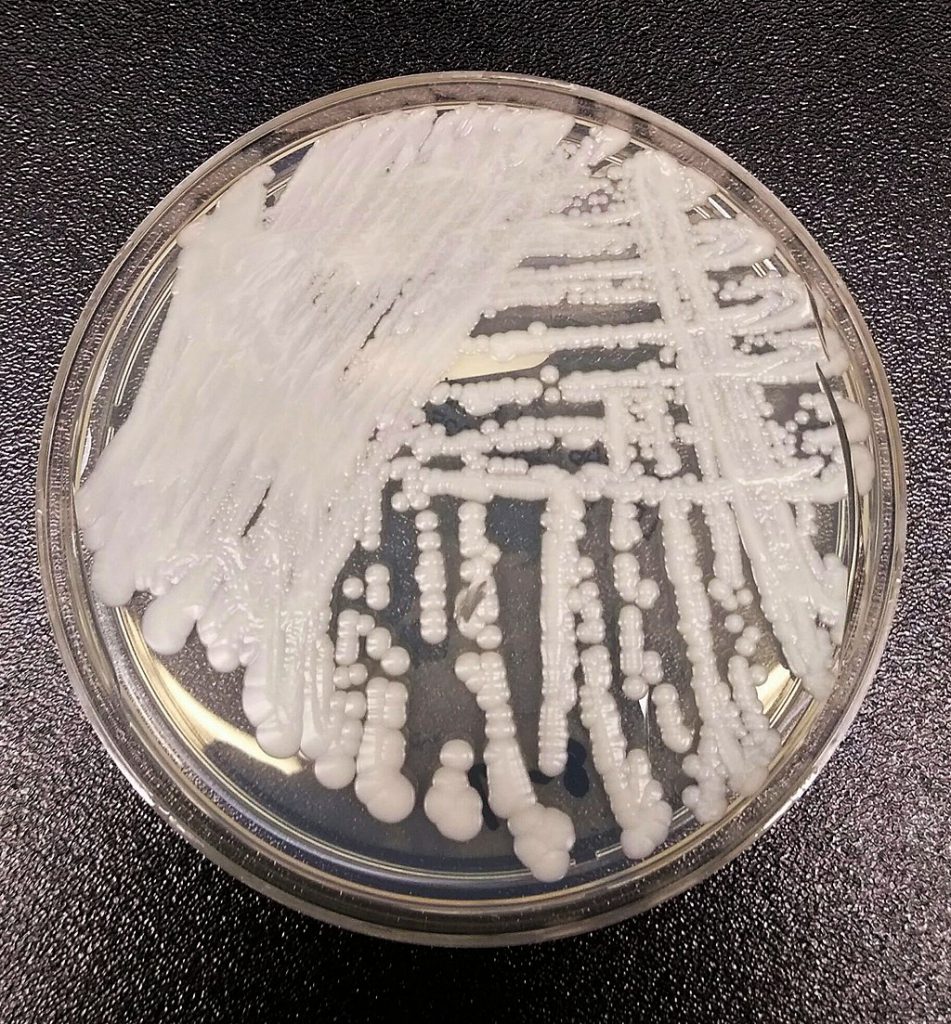
For the past five years, health officials across the world have turned an eye toward a mysterious and deadly fungus called Candida auris. With reports of the fungus reaching the United States in increasing numbers, nursing homes are under scrutiny. Many sources consider nursing homes a “breeding ground” for the fatal fungus and infection.
Nursing Home Abuse Center offers information about the fungus and infection, as well as helpful information if you or someone you love is in a hospital or nursing home.
What is Candida auris?
Candida auris is a type of fungus in the yeast family. It was first discovered in 2009 in Japan, but has since spread across the globe. The Centers for Disease Control and Prevention (CDC) reports the first known strain was identified in 1996 in South Korea. It has since been identified in Venezuela, Spain, the U.K., India, Pakistan, and South Africa.
Most recently, Candida auris was identified at Mount Sinai Hospital in Brooklyn, New York. In almost every case, the patient has been isolated to prevent spreading the fungus. Unfortunately, there are reports of unit-wide outbreaks in hospitals.
The fungus is most common in hospitals or nursing homes, with infections primarily in people with weak immune systems. Once the fungus develops, it can enter the bloodstream before spreading throughout the body. The result is a serious infection that is often fatal.
What are the Dangers of Candida auris?
The CDC is tracking cases of Candida auris, and continues to provide information to healthcare providers and families as it is available. The organization lists several concerns related to Candida auris, including:
- Unlike other forms of Candida, Candida auris is resistant to most types of antifungal medications.
- Standard laboratory methods often do not identify Candida auris. Misidentification may cause hospitals and nursing homes to improperly manage infections.
- Candida auris appears to spread easily. It has already caused outbreaks in healthcare settings across the world.
- Candida auris can infect numerous parts of the body. It is linked to ear infections, bloodstream infections and wound infections. The CDC says it may also cause bladder and lung infections.
- In hospital rooms housing patients with Candida auris, tests have revealed the fungus to be everywhere in the room, including on floor and ceiling tiles.
- The CDC believes that continued overuse of antibiotics and antifungal medications is contributing to the rise in resistant pathogens like Candida auris.
Candida auris in U.S. Nursing Homes
So far, there are at least 800 reports of infection since the fungus was first discovered in the U.S. Around half of the patients diagnosed with Candida auris infection died within 90 days. Of course, health officials are reasonably concerned. In September 2019, a nursing home resident in Brooklyn was diagnosed with Candida auris. An additional 38 patients in Palm Gardens Center for Nursing and Rehabilitation either have been diagnosed, or carry the fungus.
Public health officials are deeply concerned about facilities like the one in Brooklyn. Struggles to contain the pathogen continue and some facilities are refusing to accept patients who have a history of Candida auris. Officials in New York say that facilities with numerous patients carrying the fungus or with an active infection are contributing to the problem. Officials in Chicago mirror this concern noting that half of nursing home patients on dedicated ventilator floors have tested positive for the fungus.
What Nursing Homes Need to Know about Candida Auris
Patients in healthcare settings appear to be most at risk for Candida auris infection. The CDC warns that patients in hospitals and nursing homes are vulnerable, especially if they have weakened immune systems, or have recently had tubes or lines in their body. More specifically, risk factors in hospitals and nursing homes include:
- Recent surgery
- Diabetes
- Central venous catheters
- Intubation tubes
- Feeding tubes
- History of antifungal medication use
- History of antibiotic use
While these risk factors relate to patients most at risk, it should be noted that Candida auris infections have been diagnosed in patients of all ages. The CDC has received reports of infection in preterm infants, as well as in elderly patients. That means that hospital patients and nursing home residents should be aware of the risks, but their friends and family members should also be made aware. Since we know that Candida auris can spread, it is important that anyone who may come in contact with the fungus take precautions.
Can Nursing Homes Prevent Infections or Outbreaks?
Nursing homes who identify patients with an infection should contact the patient’s healthcare provider immediately. If the patient receives a diagnosis of Candida auris infection, caregivers must be diligent in following treatment guidelines.
Most patients will receive antifungal drugs, and some may receive antibiotics. Unfortunately, as noted before, this particular fungus is resistant to most of these medications. Often, patients must endure several rounds of various high-dose antifungal medications in order for the fungus to be eradicated.
As for preventing the spread of Candida auris, the CDC recommends nursing homes and hospitals do the following:
- Place the patient in a single-person room.
- Use Standard and Contact precautions when entering and exiting the room.
- Adhere to hand hygiene practices.
- Clean and disinfect all patient care instruments, reusable equipment and the patient environment.
- Communicate carefully about the patient’s diagnosis if he or she moves to a different facility.
- Minimize the number of staff members who come into contact with the infected patient.
- If there are multiple patients with the infection, considering assigning the same staff members to those patients to reduce the risk of transmission.
All of these infection control measures are important to prevent Candida auris from causing an outbreak. However, the CDC notes that patients may be colonized with the fungus for several months after the infection. That means they could be at risk for future infection. Consequently, ongoing infection control in nursing homes is paramount to preventing the spread of this dangerous infection.
Sources:
- https://www.nytimes.com/2019/09/11/health/nursing-homes-fungus.html
- https://www.nytimes.com/2019/04/06/health/drug-resistant-candida-auris.html?module=inline
- https://www.nytimes.com/2019/04/17/health/candida-auris-fungus-chicago.html?module=inline
- https://www.cdc.gov/fungal/candida-auris/candida-auris-qanda.html
- https://www.cdc.gov/fungal/candida-auris/c-auris-infection-control.html


