Nursing Homes and COVID-19
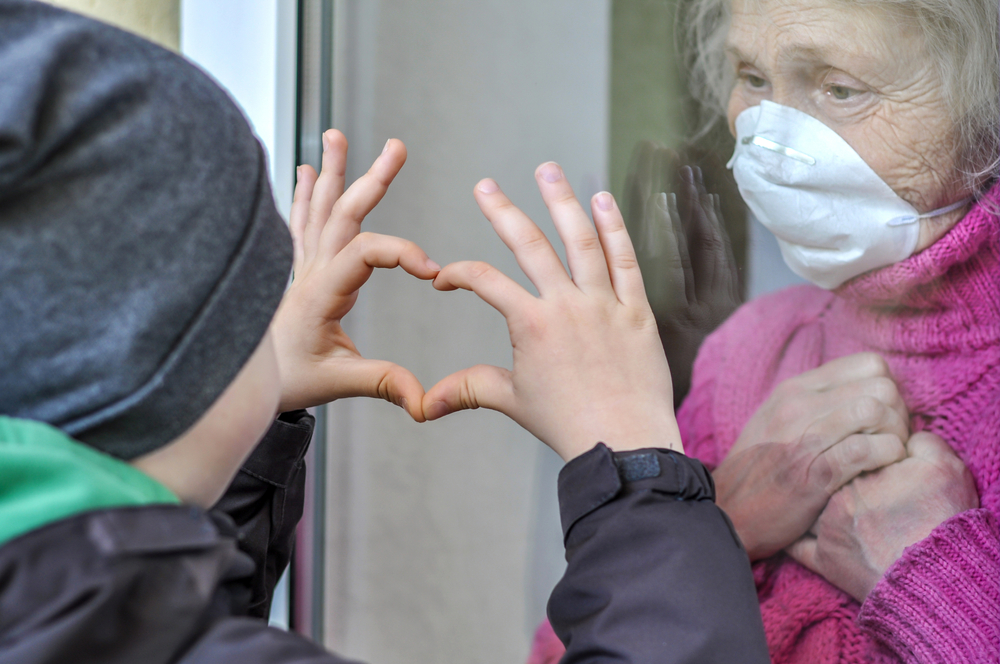
The novel coronavirus, COVID-19, continues to cause fear among Americans. The widespread fear is no greater among any group than it is for residents and staff in nursing homes. There are hundreds of outbreaks of coronavirus in nursing homes across the United States. These outbreaks are causing residents, staff and family members overwhelming concern about their safety and the future.
The nursing home abuse lawyers at Fight Nursing Home Abuse are already receiving calls from family members who are concerned about loved ones who live in a nursing home. Family members are concerned about the level of care and attention that their loved ones are receiving, infection control in nursing homes and when they may be able to visit their loved ones again.
Fight Nursing Home Abuse hopes to help families get some answers to these questions and more. Read on to learn more about coronavirus in nursing homes. Also, you can call us at 1-866-548-9636 if you have questions or concerns.
What is Coronavirus?
A coronavirus is a virus or disease that spreads from animals to humans. A novel coronavirus, like COVID-19, is a new coronavirus that has not been identified before in the world. The coronavirus that is currently affecting the entire world is not the same kind of virus that causes mild illnesses. Instead, COVID-19 affects the lungs and can cause serious damage and complications.
Many people who contract COVID-19 experience mild symptoms like fever, cough and shortness of breath. However, the elderly, people with weak immune systems and people with underlying health conditions are susceptible to more serious illness and complications. Among these individuals, symptoms may worsen quickly with difficulty breathing and chest pain being the most common complaints.
The World Health Organization (WHO) calls COVID-19 a global pandemic. The virus has reached more than 170 countries across the world, causing more than 2.4 million illnesses. More than 165,000 people have died as a result of the virus or related complications. Sadly, the majority of people who have died are elderly or lived in a nursing home.
The Spread of Coronavirus in Nursing Homes
COVID-19 primarily spreads through respiratory droplets. That means when someone who has the virus coughs or sneezes, those droplets of bodily fluid carry the virus to anyone, or any surface, nearby. If someone inhales these particles, then they may contract the coronavirus. Similarly, if someone touches an item that is contaminated and then touches their face, they may also contract the virus.
In nursing homes, residents and staff members are vulnerable to the spread of the coronavirus for several reasons. Primarily:
Nursing Home Residents:
- Are elderly
- Have underlying medical conditions
- Share confined quarters
- Share public areas with other residents, staff and visitors
Nursing Home Staff:
- Directly attend residents who may have the coronavirus
- Clean areas that may be contaminated
- Shares public areas with residents and visitors
Healthcare experts call these factors a “perfect storm” for virus spread. These factors are why hygiene and infection control in nursing homes are so important.
How Many Nursing Homes are Affected by Coronavirus?
State Health Departments are responsible for reporting cases of COVID-19 in nursing homes. Unfortunately, testing delays and delays in reporting make it difficult to know just how many nursing homes are affected. Data that is currently available shows:

What are Nursing Homes Required to Do to Stop the Spread?
We have all heard that preventing the spread of the coronavirus is similar to preventing the spread of the flu. Frequent hand-washing, monitoring symptoms, eating healthy and avoiding people who are sick are all recommended. This is certainly important to prevent the spread of coronavirus in nursing homes.
Nursing homes are also required to meet certain infection control guidelines. These guidelines include specific precautions that facilities can take to avoid an outbreak. The Centers for Medicare & Medicaid Services (CMS) infection control guideline §483.65 says,
“The facility must establish and maintain an Infection Control Program designed to provide a safe, sanitary and comfortable environment and to help prevent the development and transmission of disease and infection.”
But is that enough? Given the continued coronavirus outbreaks in nursing homes, the answer would seem to be “no.”
Coronavirus Guidelines
In addition to standard guidelines and recommendations, CMS and the Centers for Disease Control and Prevention (CDC) established more specific guidelines designed to prevent the spread of coronavirus in nursing homes. These guidelines include:
- Restricting visitation for all non-essential healthcare providers and staff members.
- Use multiple means of notifying non-essential visitors and family members of visitation restrictions.
- If a facility allows visitors for end-of-life care, they should enforce hand hygiene and use of Personal Protective Equipment (PPE), including face masks.
- Provide instructions to any allowed visitors on proper hand hygiene, use of PPE and limiting touching of surfaces.
- Visitors who have a fever or respiratory symptoms should not be allowed in the facility for any reason.
- Facilities should consider implementing alternatives to regular visits for family members, such as:
- Virtual communication (phone, video chat, etc.)
- Using a listserv communication method to update families
- Assigning certain staff members as contacts for family members
- Implementing a voice recorded phone line families can use for regular updates
- Implement active screening procedures for all residents and staff. Screen for fever and respiratory symptoms.
- All communal dining and activities should be cancelled.
- Remind residents and staff to use proper hand hygiene.
- Staff members who are sick should wear a face mask and self-isolate at home.
- Staff members who work at more than one facility should be screened at each location prior to entry.
- Facilities should review their policies for interacting with vendors and revise as necessary. This includes policies related to receiving supplies, EMS personnel, transportation services and non-healthcare providers.
- Facilities should consider dedicating a unit or wing to residents who are returning from the hospital, so they can be quarantined for 14 days before re-entering the community setting.
Inadequate Infection Control in Nursing Homes
At Nursing Home Abuse Center, we are receiving reports related to coronavirus in nursing homes. These reports include nursing homes running out of supplies, including antibacterial agents and face masks. Some reports also relate to staffing shortages due to stay-at-home or shelter in place orders, or staff members being sick. These reports certainly suggest that most nursing homes were not prepared to handle an outbreak.
Furthering the idea that nursing homes are woefully unprepared for an outbreak like this one is the fact that many nursing homes battling outbreaks have a history of deficiencies with federal and state infection control guidelines. Currently, more than 660 Medicare-certified nursing homes across the U.S. report cases of coronavirus. Of those, 40 percent have been cited at least once for deficiencies in infection control in the past few years.
These numbers are truly unacceptable. Nursing homes have a legal responsibility to follow health and safety guidelines and ensure the health and safety of their residents.
Guidelines for Infection Control in Nursing Homes
CMS has specific infection control guidelines that nursing homes must adhere to at all times – not just during a global pandemic. These guidelines include infection control measures, such as:
- Investigating, controlling and preventing infections.
- Deciding if individual residents need to be isolated. Residents with “droplet precautions,” such as those testing positive for COVID-19, should be isolated.
- Maintaining record of incidents and corrective action taken in response to an infection.
- To prevent the spread of infection, residents who test positive must be isolated.
- If a staff member has a communicable disease or infection, he or she must not have direct contact with residents or food if transmission is likely.
- Staff members must observe accepted professional hand washing practices after direct contact with any resident.
- Staff members must be provided with adequate Personal Protective Equipment (PPE) when handling items containing bodily fluids or infectious fluids.
- If an infection is airborne, staff members should wear a face mask or respirator when working with residents.
- Staff must handle linens in such a way as to prevent the spread of infection.
- If a facility recognizes the potential for an outbreak, then it must take appropriate steps to contain it.
Have Questions about Coronavirus in Nursing Homes?
Do you have questions about coronavirus in nursing homes? Are you concerned that your loved one is not getting the quality care that he or she deserves? If so, contact Fight Nursing Home Abuse to speak with one of our nursing home abuse lawyers about your situation. Nursing homes can be held liable for harm that residents suffer due to negligence. In the case of coronavirus, such negligence may include:
- Failing to follow state, CDC and CMS COVID-19 guidelines
- Continuing practices that could promote further spread of COVID-19
- Failing to test patients and staff members with symptoms
- Failing to isolate residents who test positive
If you have concerns about any of these deficiencies, contact us. Find out how we can help you protect your loved one and his or her legal rights. If the nursing home is negligent, you may have an actionable legal claim. You may also be able to pursue compensation for the harm your loved one has experienced.
Find out more by contacting Fight Nursing Home Abuse at 1-866-548-9636. We offer free consultations to every potential client.
Sources:
- https://www.who.int/emergencies/diseases/novel-coronavirus-2019
- https://www.cdc.gov/coronavirus/2019-ncov/index.html
- https://www.cdc.gov/coronavirus/2019-ncov/hcp/long-term-care.html
- https://www.cms.gov/files/document/qso-20-14-nh-revised.pdf
- https://www.cms.gov/Regulations-and-Guidance/Guidance/Transmittals/downloads/r55soma.pdf


